

Cayson Sanderford sometimes gets in trouble at school for being active, and his parents couldn’t be happier.
Having plenty of energy is a sign that Cayson’s heart is working well.
Now a 6-year-old first-grader from Mathiston, Cayson is the first patient at UMMC to undergo one of the most complicated heart surgeries, known as the Norwood procedure. It is the first of at least three surgeries to correct the congenital heart defect called hypoplastic left heart syndrome, which occurs when the left side of the heart fails to develop correctly. At the time of the surgery, Cayson was 10 days old.
“Before any of this happened, I knew nothing about hypoplastic left heart syndrome,” said his mom, Stephanie Sanderford. “I had no idea what the Norwood was. I had no idea he was the first patient to have that surgery at Batson Children’s Hospital. I think it is good that we didn’t know at the time, because if we did, we might have been in a tailspin.”

In hypoplastic left heart syndrome, the left side of the heart can’t effectively pump blood to the body, so the right side of the heart must pump blood both to the lungs and to the rest of the body. If left untreated, hypoplastic left heart syndrome is fatal.
About one in every 100 babies born has some form of congenital heart defect. Of those, less than 5 percent are born with hypoplastic left heart syndrome.
Cayson’s congenital heart defect was missed in ultrasound readings, Sanderford said. She and husband Jason, after undergoing invitro fertilization, were thrilled to become parents.
“The whole pregnancy, everything looked great,” she said.
Cayson’s ashen color was the first sign of trouble, but that was initially blamed on a long delivery, some 26 hours, and he went home the next day.
Sanderford said she noticed, shortly after taking her newborn son home from the hospital, that he was breathing heavily. “At first I thought I was just being paranoid. I’ve never been a parent before,” she said.
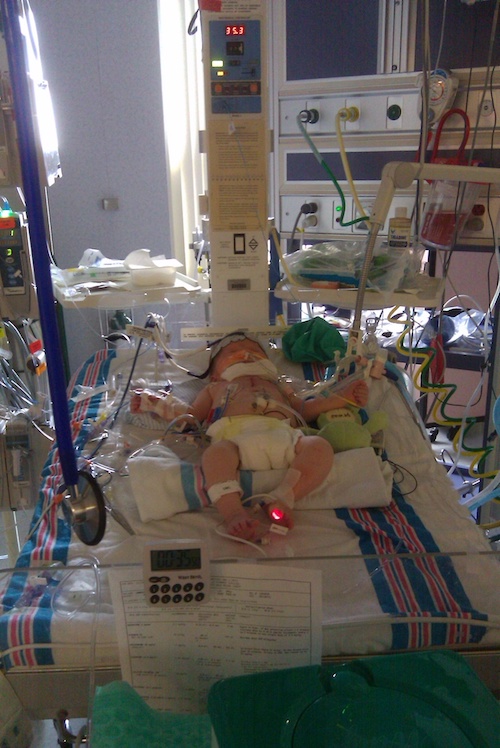
Then, Cayson’s symptoms grew worse. He wasn’t eating and was struggling to breathe. A trip to the family’s local emergency room turned into an ambulance ride to Batson Children’s Hospital.
There, they met with Dr. Avichal Aggarwal, assistant professor of pediatric cardiology at UMMC.
“I remember asking the doctor what was happening, and he told me that his condition was as serious as it could get. We were scared and just shocked,” Sanderford said in a news story about the Norwood surgery in 2011.
“He came in at 3 in the morning when we got to Batson,” Sanderford remembered. “Dr. Aggarwal had come home from the hospital at midnight and had gotten a call about Cayson. He said that something told him to get up out of bed and come to the hospital to check it out then rather than waiting until morning. We are so thankful he did that!”
“I remember that night very well,” said Aggarwal. “Cayson’s parents were in tears, and I had to tell them he’d need a minimum of three surgeries to get to a normal set of vital signs. They were thinking that the feeding problem was something like reflux, so learning Cayson was born with a heart defect was a shock for them.”
He has since had other surgeries – the Glenn procedure at 5 months, the Fontan at 18 months and a fenestration closure 10 days after the Fontan. He visits Aggarwal for follow-up cardiac care.
“He is the best,” said Sanderford. “We love him!”

Aggarwal feels the same way about the Sanderfords. “You get very attached to families because you go through these surgeries together. You bond.”
Children born with hypoplastic left heart syndrome are not cured by surgery, Aggarwal said. “They will need lifelong follow-up care to monitor their health.”
Since his surgeries, not much slows Cayson down these days.
Cayson is “all boy,” Sanderford said. “He played tee-ball this summer and, before that, played buddy ball. He’s finished kindergarten and would get in trouble because he couldn’t stay still and would play too rough on the playground, which is great for parents of a child born with a heart defect to hear. He keeps up with everyone his age, and his favorite thing to do is run and race.”
Story and photos by University of Mississippi Medical Center
Recent Comments